Journal Description
Infectious Disease Reports
Infectious Disease Reports
is an international, peer-reviewed, open access journal on infectious diseases published bimonthly online by MDPI (since Volume 12, Issue 3 - 2020).
- Open Access— free for readers, with article processing charges (APC) paid by authors or their institutions.
- High Visibility: indexed within Scopus, ESCI (Web of Science), PubMed, PMC, Embase, and other databases.
- Rapid Publication: manuscripts are peer-reviewed and a first decision is provided to authors approximately 34.1 days after submission; acceptance to publication is undertaken in 5.1 days (median values for papers published in this journal in the second half of 2025).
- Journal Rank: CiteScore - Q2 (Infectious Diseases)
- Recognition of Reviewers: APC discount vouchers, optional signed peer review, and reviewer names published annually in the journal.
- Benefits of Publishing: We aim to be a leading journal on infectious diseases and to be in the top 20 journals listed in the Journal Citation Report (JCR) in this specific category in the near future.
Impact Factor:
2.4 (2024);
5-Year Impact Factor:
2.2 (2024)
Latest Articles
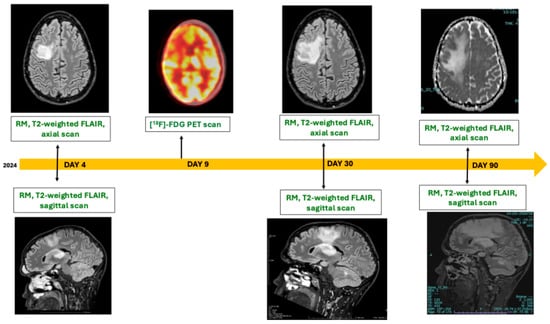
Progressive Multifocal Leukoencephalopathy in AIDS: The Diagnostic Role of PET Imaging
Infect. Dis. Rep. 2026, 18(2), 33; https://doi.org/10.3390/idr18020033 - 8 Apr 2026
Abstract
►
Show Figures
Introduction: The majority of progressive multifocal leukoencephalopathy (PML) cases is still represented by patients affected by acquired immunodeficiency syndrome (AIDS). Diagnosis of PML relies on histopathological findings or by the combination of clinical signs, radiological evidence, and molecular positivity of the JC virus
[...] Read more.
Introduction: The majority of progressive multifocal leukoencephalopathy (PML) cases is still represented by patients affected by acquired immunodeficiency syndrome (AIDS). Diagnosis of PML relies on histopathological findings or by the combination of clinical signs, radiological evidence, and molecular positivity of the JC virus in cerebrospinal fluid. However, AIDS status predisposes to various diseases involving the brain, testing the diagnostic ability of the clinician. Case description: We describe a PML case in a patient with AIDS, in whom lumbar puncture was initially impossible for severe thrombocytopenia and magnetic resonance showed an hyperintense lesion and was unable to distinguish between PML and lymphoma. In this case, [18F]-fluorodeoxyglucose (FDG)-PET imaging showing a hypometabolism of the lesion helped to initially orient toward PML, as diagnosis was later confirmed by lumbar puncture. We collected 21 cases in the literature in which [18F]-FDG-PET was helpful in cases of PML. Discussion and Conclusions: PET imaging is not considered a standard diagnostic tool for PML. However, in selected cases, it may provide valuable information to direct the diagnosis towards PML.
Full article
Open AccessCase Report
Brucella anthropi Endocarditis: An Unusual Pathogen
by
Fernando Baires, Erin Arias, María José Díaz, Cesar Burgos, Carlos A. Umaña Mejia, Justice Cruz, Joanne Cordero Guerra, Helen Hoffman, Jack Bordovsky, Jana Radwanski, Miguel Sierra-Hoffman and Amy C. Madril
Infect. Dis. Rep. 2026, 18(2), 32; https://doi.org/10.3390/idr18020032 - 8 Apr 2026
Abstract
►▼
Show Figures
Background: The genus Brucella has expanded considerably in the 21st century. With the advent of advanced phylogenetic analyses, a close genetic relationship between Brucella and Ochrobactrum has been identified, leading to reclassification of Ochrobactrum species within the genus Brucella. Among these, Brucella
[...] Read more.
Background: The genus Brucella has expanded considerably in the 21st century. With the advent of advanced phylogenetic analyses, a close genetic relationship between Brucella and Ochrobactrum has been identified, leading to reclassification of Ochrobactrum species within the genus Brucella. Among these, Brucella anthropi (formerly Ochrobactrum anthropi) is increasingly recognized as a rare cause of invasive human infection. We report a clinically significant case of B. anthropi infective endocarditis and review the available literature. Methods: We report a case of B. anthropi infective endocarditis and conducted a narrative review of the English-language medical literature through 2025. Cases were analyzed for demographics, clinical presentation, antimicrobial susceptibility, and outcomes. Results: A 75-year-old man with a prosthetic aortic valve and prior endocarditis presented with fever of unknown origin, weight loss, and prior transient ischemic attacks. Blood cultures grew B. anthropi after prolonged incubation. Transesophageal echocardiography demonstrated vegetations involving both the aortic and tricuspid valves, and the patient required targeted combination antimicrobial therapy due to persistent bacteremia. Seven additional cases of B. anthropi infective endocarditis were identified on review of the literature. Most patients had underlying valvular disease or prosthetic material. Reported lethality approached 25%. Antimicrobial susceptibility patterns were variable, underscoring the importance of targeted individualized therapy. Conclusion: Consistent with other Gram-negative bacilli, B. anthropi is a rare but established cause of acute bacterial endocarditis. Despite its rarity, it may represent an under-recognized cause of invasive disease. This case highlights the importance of prolonged culture incubation, careful microbiologic interpretation, and susceptibility-guided therapy.
Full article

Figure 1
Open AccessReview
Therapeutic Management of Septic Venous Thrombosis: A Narrative Review
by
Anabel Franco-Moreno, Ana Bustamante-Fermosel, Juan Torres-Macho and Belén Comeche-Fernández
Infect. Dis. Rep. 2026, 18(2), 31; https://doi.org/10.3390/idr18020031 - 3 Apr 2026
Abstract
Background/Objectives: Septic venous thrombosis is an uncommon complication but clinically significant due to its high morbidity and mortality and the complexity of therapeutic decision-making. The lack of standardized guidelines and the scarcity of high-quality studies complicate clinical management, as most available evidence derives
[...] Read more.
Background/Objectives: Septic venous thrombosis is an uncommon complication but clinically significant due to its high morbidity and mortality and the complexity of therapeutic decision-making. The lack of standardized guidelines and the scarcity of high-quality studies complicate clinical management, as most available evidence derives from highly heterogeneous case series and retrospective studies. In this context, a comprehensive overview is essential to guide real-world practice. Methods: This manuscritp provides an in-depth review of the treatment of septic venous thrombosis at its most frequent sites, including the portal vein and its branches, the pelvic veins, catheter-associated events, the internal jugular vein, and dural venous sinus thrombosis. Results: Across all scenarios, early initiation of appropriate antibiotic therapy is the cornerstone of treatment and must be tailored to the suspected source of infection and the patient’s clinical course. In parallel, although the role of anticoagulation remains debated, several observational studies suggest potential benefits in terms of recanalization and complication prevention, particularly in selected patients. Conclusions: However, the decision to anticoagulate should be carefully individualized within a multidisciplinary framework. Despite the recent progress, many clinical uncertainties remain. Therefore, well-designed clinical trials are needed to define optimal therapeutic strategies for this condition.
Full article
(This article belongs to the Special Issue Review on Infectious Diseases)
►▼
Show Figures

Figure 1
Open AccessCase Report
Non-Typhoidal Salmonella enterica Bacteremia Complicated by Native Shoulder Septic Arthritis in a Patient with Sickle Cell Disease Following Foodborne Exposure: A Case Report and Literature Review
by
Gabriel A. Godart, Vidit Yadav, Joseph M. Bestic, Bradley S. Schoch, Bryan D. Springer, Ravi V. Durvasula, Sammer M. Elwasila and Justin M. Oring
Infect. Dis. Rep. 2026, 18(2), 30; https://doi.org/10.3390/idr18020030 - 2 Apr 2026
Abstract
Background/Objectives: Non-typhoidal Salmonella (NTS) species are well-recognized causes of invasive infection in patients with sickle cell disease (SCD), with a particular predilection for the musculoskeletal system. Although Salmonella osteomyelitis is well described in this population, septic arthritis is uncommon, especially involving the shoulder
[...] Read more.
Background/Objectives: Non-typhoidal Salmonella (NTS) species are well-recognized causes of invasive infection in patients with sickle cell disease (SCD), with a particular predilection for the musculoskeletal system. Although Salmonella osteomyelitis is well described in this population, septic arthritis is uncommon, especially involving the shoulder joint. We describe a case of NTS bacteremia complicated by native shoulder septic arthritis in a patient with SCD and review its clinical implications. Methods: We report the clinical course, diagnostic evaluation, microbiologic findings, imaging studies, and management of a 22-year-old man with homozygous SCD who presented with a vaso-occlusive pain crisis and subsequently developed severe sepsis with persistent Salmonella enterica bacteremia following ingestion of undercooked poultry. Persistent bacteremia prompted further evaluation for metastatic infection using advanced imaging and diagnostic arthrocentesis. Results: Whole-body imaging identified septic arthritis of the native right shoulder, which was confirmed by synovial fluid cultures growing Salmonella species. The patient underwent arthroscopic irrigation and debridement for source control. Antimicrobial therapy was narrowed to intravenous ceftriaxone based on susceptibility data and continued for six weeks. The patient demonstrated clinical improvement with resolution of bacteremia and was discharged to rehabilitation to complete therapy. Conclusions: This case highlights the importance of a careful exposure history, including foodborne sources, in patients with SCD presenting with invasive Salmonella infection. Persistent bacteremia should prompt early investigation for metastatic foci, and timely surgical source control combined with targeted antimicrobial therapy is essential for optimal outcomes in this population.
Full article
(This article belongs to the Section Bacterial Diseases)
►▼
Show Figures

Figure 1
Open AccessArticle
A Blood-Based Interferon Viral Score Defines Acute RSV Bronchiolitis in Infants
by
Ilaria Galliano, Stefania Alfonsina Liguori, Anna Pau, Paola Montanari, Cristina Calvi, Anna Clemente, Anna Massobrio, Claudia Linari, Stefano Gambarino, Alessandra Conio and Massimiliano Bergallo
Infect. Dis. Rep. 2026, 18(2), 29; https://doi.org/10.3390/idr18020029 - 1 Apr 2026
Abstract
►▼
Show Figures
Background: Respiratory syncytial virus (RSV) is the leading cause of bronchiolitis and hospitalization in infancy. Reliable biomarkers reflecting host antiviral responses and disease dynamics are still lacking. Methods: We evaluated the expression of the interferon-stimulated genes IFI44L, IFI27, and RSAD2 in peripheral blood
[...] Read more.
Background: Respiratory syncytial virus (RSV) is the leading cause of bronchiolitis and hospitalization in infancy. Reliable biomarkers reflecting host antiviral responses and disease dynamics are still lacking. Methods: We evaluated the expression of the interferon-stimulated genes IFI44L, IFI27, and RSAD2 in peripheral blood of infants hospitalized with RSV bronchiolitis at admission and discharge, and in healthy controls, using multiplex RT-qPCR. A composite interferon-based Viral Score was derived from coordinated ISG expression. Results: All three ISGs and the Viral Score were markedly elevated during acute RSV infection at hospital admission compared with discharge and healthy controls. Following clinical recovery, ISG expression and Viral Score declined significantly and approached baseline levels. The Viral Score clearly discriminated acute infection from recovery and healthy states, reflecting dynamic systemic interferon activation. Conclusions: A Viral Score based on IFI44L, IFI27, and RSAD2 captures systemic antiviral immune responses in infants with RSV bronchiolitis and declines with disease resolution. This interferon-based host-response signature represents a promising biomarker for defining viral infection status and monitoring disease dynamics in pediatric respiratory infections.
Full article

Figure 1
Open AccessEditor’s ChoiceArticle
Heart Failure Incidence and Risk Factors in U.S. Adults Receiving Bezlotoxumab: A Large Database Analysis
by
Chia-Yu Chiu, Daniel B. Chastain, Joseph Sassine and Andrés F. Henao-Martínez
Infect. Dis. Rep. 2026, 18(2), 28; https://doi.org/10.3390/idr18020028 - 31 Mar 2026
Abstract
Background: Bezlotoxumab is used to prevent recurrent Clostridioides difficile infection. Although well tolerated, heart failure (HF) exacerbations have been reported as adverse events in clinical trials. This study evaluates the incidence and predictors of HF exacerbation following bezlotoxumab. Methods: We used the TriNetX
[...] Read more.
Background: Bezlotoxumab is used to prevent recurrent Clostridioides difficile infection. Although well tolerated, heart failure (HF) exacerbations have been reported as adverse events in clinical trials. This study evaluates the incidence and predictors of HF exacerbation following bezlotoxumab. Methods: We used the TriNetX research database to identify U.S. adults who received bezlotoxumab and stratified them into three groups based on HF history: no HF, HF with preserved ejection fraction (HFpEF), and HF with reduced ejection fraction (HFrEF). The 90-day cumulative incidence of HF events and mortality were assessed. Cox proportional hazard models identified predictors of HF events. Results: Among 2515 patients, 89% had no HF history, 4% had HFpEF, and 7% had HFrEF. The 90-day HF event rates were 1%, 29%, and 52% for the no HF, HFpEF, and HFrEF groups, respectively (p < 0.001). The 90-day all-cause mortality was 0.9%. Corresponding 90-day all-cause mortality rates were 0.04%, 4%, and 11%, respectively (p < 0.001). Independent positive predictors of HF events included HFrEF (aHR 19.400), HFpEF (adjusted hazard ratio [aHR] 8.632), heart transplant (aHR 7.485), hyperlipidemia (aHR 3.184), valvular heart disease (aHR 2.267), chronic kidney disease stage ≥ 3 (aHR 1.715), and ischemic heart disease (aHR 1.987). Protective factors included non-cardiac solid organ transplant (aHR 0.333). Conclusions: Bezlotoxumab appears safe in patients without HF history but is associated with a significantly increased risk of HF exacerbation in those with pre-existing HF, especially HFrEF.
Full article
(This article belongs to the Section Bacterial Diseases)
►▼
Show Figures

Figure 1
Open AccessArticle
Matrix-Dependent Sensitivity of Two Pan-Trematode PCR Assays for Detecting Schistosoma spp. in Clinical Human Samples
by
Hagen Frickmann, Andreas Hahn, Kirsten Alexandra Eberhardt, Ulrike Loderstädt, Norbert Georg Schwarz and Ralf Matthias Hagen
Infect. Dis. Rep. 2026, 18(2), 27; https://doi.org/10.3390/idr18020027 - 27 Mar 2026
Abstract
Background: Schistosoma spp. are trematodes occurring in tropical endemic areas but can be imported to non-endemic regions as causes of travel-associated infections. In this study, two pan-trematode-specific real-time PCR assays were evaluated for their diagnostic sensitivity in detecting Schistosoma spp. DNA in diagnostic
[...] Read more.
Background: Schistosoma spp. are trematodes occurring in tropical endemic areas but can be imported to non-endemic regions as causes of travel-associated infections. In this study, two pan-trematode-specific real-time PCR assays were evaluated for their diagnostic sensitivity in detecting Schistosoma spp. DNA in diagnostic human samples. Methods: Two previously described pan-trematode-specific real-time PCR assays were comparatively assessed using diagnostic samples containing DNA of either the S. haematobium complex or the S. mansoni complex, as confirmed by Schistosoma species complex-specific real-time PCR. Results: Out of a total of 655 samples containing Schistosoma spp. DNA, positive signals in at least one of the two pan-trematode real-time PCR assays were recorded for 17 (2.6%) nucleic acid extractions. Although sensitivity was in the >90% range for stool samples, only a few individual blood plasma and serum samples, and none of the Schistosoma spp. DNA-containing tissue or urine samples, tested positive by pan-trematode PCR. The lower sensitivity of pan-trematode PCR compared with Schistosoma spp.-specific PCR was semi-quantitatively confirmed by higher cycle threshold (Ct) values in the former. When comparing samples with concordant versus discordant positive results for Schistosoma spp.-specific and pan-trematode PCR, Ct values of the Schistosoma spp.-specific PCR were lower in concordantly positive samples than in discordantly positive samples. Conclusions: While the assessed pan-trematode PCR assays showed insufficient sensitivity as screening tools for blood plasma, blood serum, tissue, and urine samples from individuals with suspected schistosomiasis, they were sufficiently sensitive when applied to stool samples, in which substantial amounts of target DNA, as indicated by low Ct values in the Schistosoma species complex-specific real-time PCR assays, can be expected. For screening for Schistosoma spp. DNA in sample materials other than stool, the use of highly sensitive target-specific PCR remains necessary.
Full article
Open AccessArticle
Comparative Molecular Docking and Pharmacokinetic Profiling of Cinnamic Acid and Oleic Acid from Cinnamomum verum as Potential Inhibitors of Dengue Virus Proteins
by
Wafaa Hussien Habeeb, Noor Hameed Hanoush, Meena Thaar Alani, Ali Hazim Abdulkareem, Mohammed Obaid Ibrahim, Mohammed Salih Al-Janaby, Mohammed Mukhles Ahmed, Saja Saadallah Abduljaleel and Zaid Mustafa Khaleel
Infect. Dis. Rep. 2026, 18(2), 26; https://doi.org/10.3390/idr18020026 - 26 Mar 2026
Abstract
Background: Dengue virus (DENV) does not have any effective antiviral therapy. The Cinnamomum verum has cinnamic acid and oleic acid that could inhibit important viral proteins. Aim: To compare their inhibitory capacity with the key DENV proteins through molecular docking, molecular dynamics and
[...] Read more.
Background: Dengue virus (DENV) does not have any effective antiviral therapy. The Cinnamomum verum has cinnamic acid and oleic acid that could inhibit important viral proteins. Aim: To compare their inhibitory capacity with the key DENV proteins through molecular docking, molecular dynamics and in silico ADMET. Methods: Phytochemical profiling of the ethanolic extract of the bark was done by GCMS. AutoDock Vina (version 1.2.0) was used to dock cinnamic acid and oleic acid to key proteins of DENV (NS5, NS3, and envelope) in the presence of ribavirin as the reference. The best complexes were then subjected to 50 ns of molecular dynamics simulation and stability measured by RMSD, RMSF, Rg, SASA, hydrogen bonding and RDF. Validated in silico tools were used to predict the ADMET properties. Results: Analysis of GC–MS revealed cinnamic acid (85.92%) and oleic acid (5.33%). The outcome of docking was that the cinnamic acid had the greatest affinity with NS5 (−5.970 kcal/mol) and the capsid protein (−5.755 kcal/mol), and oleic acid showed the highest affinity with the capsid (−6.150 kcal/mol) and then with NS5 (−5.209 kcal/mol). Both ligands had a relatively weak interaction with NS3. Simulation of the molecular dynamics showed the stability of the top complexes, especially the cinnamic acid–NS5 complex, that retained low RMSD (1.6–1.9 A), stable Rg and SASA profiles, and continued hydrogen bonding during the 50 ns period. The use of cinnamic acid in ADMET projections was more preferable, as it was more soluble, orally bioavailable (0.91), and drug-like (QED 0.65), but oleic acid revealed higher lipophilicity and lower drug-like properties (QED 0.29). Conclusions: Cinnamic acid showed specificity towards the NS5 proteins with the help of stable dynamics and good predicted pharmacokinetics, which are features that make it a promising multi-target anti-DENV scaffold. Oleic acid exhibited poor affinity and poor pharmacokinetic properties. The findings are predictive and must be validated using biochemical, cellular, and toxicological means to prove the antiviral efficacy and safety.
Full article
(This article belongs to the Special Issue Epidemiology, Prevention and Research on Dengue Virus)
►▼
Show Figures

Figure 1
Open AccessSystematic Review
Global Review on Naegleria fowleri Cases: Contemporary Epidemiology, Diagnosis, Treatment and Outcomes
by
Andreas Sarantopoulos, Annalisa Quattrocchi, Ioannis Kopsidas, Oliver A. Cornely, Danila Seidel, Itamar Grotto and Zoi Dorothea Pana
Infect. Dis. Rep. 2026, 18(2), 25; https://doi.org/10.3390/idr18020025 - 24 Mar 2026
Abstract
►▼
Show Figures
Background/Objectives: Primary amoebic meningoencephalitis (PAM) is a rare, fulminant, and often fatal central nervous system infection caused by the opportunistic free-living amoeba Naegleria fowleri. Although Naegleria species are widely present in freshwater and soil worldwide, human disease is associated specifically with pathogenic
[...] Read more.
Background/Objectives: Primary amoebic meningoencephalitis (PAM) is a rare, fulminant, and often fatal central nervous system infection caused by the opportunistic free-living amoeba Naegleria fowleri. Although Naegleria species are widely present in freshwater and soil worldwide, human disease is associated specifically with pathogenic N. fowleri rather than the many nonpathogenic environmental species, and virulence may vary across N. fowleri isolates. This systematic review aimed to synthesize contemporary global data from 2000 to 2024 to identify recent trends in epidemiology, clinical presentation, diagnosis, treatment, and outcomes. Methods: A systematic literature search was conducted across PubMed, Scopus, and the Cochrane Library, identifying 58 eligible publications encompassing 66 individual cases. Results: Most reports originated from the United States, India, and China. The median patient age was 14 years, with 78% of cases occurring in males. Annual case reports increased from one per year (2000–2005) to over four per year (2020–2024), reflecting either a true rise in incidence or improved detection. Common presenting symptoms included fever, headache, and altered mental status. Diagnosis was confirmed via polymerase chain reaction (PCR) testing or post-mortem biopsy in nearly one-third of cases. Treatment regimens varied, with amphotericin B and miltefosine being the most frequently used agents. Overall mortality was 83%, with survival strongly associated with early initiation of combination therapy. Pediatric patients had a higher survival rate (22%) compared to adults (7.1%). Conclusions: The findings highlight the need for heightened clinical awareness, especially in the context of climate-driven ecological changes that may expand N. fowleri’s geographic range. This review underscores critical gaps in surveillance and diagnostics and emphasizes the importance of a One Health approach to addressing emerging threats like PAM. Further research into novel therapeutics, rapid diagnostics, and global case reporting systems is urgently needed.
Full article

Figure 1
Open AccessArticle
Clinical Management of Severe Cupriavidus gilardii Superinfection After Influenza a Virus Pneumonia: A Case Report and Literature Review
by
Chenxia Guo, Cuihong Sun, Jiajia Zheng, Qingtao Zhou and Ying Liang
Infect. Dis. Rep. 2026, 18(2), 24; https://doi.org/10.3390/idr18020024 - 13 Mar 2026
Abstract
Background: Cupriavidus is an aerobic Gram-negative bacterium and a rare conditional pathogen that mainly infects immunocompromised patients or those undergoing invasive procedures. Methods: We present the case of a 70-year-old male with diabetes mellitus who developed septic shock following influenza A virus (IAV)
[...] Read more.
Background: Cupriavidus is an aerobic Gram-negative bacterium and a rare conditional pathogen that mainly infects immunocompromised patients or those undergoing invasive procedures. Methods: We present the case of a 70-year-old male with diabetes mellitus who developed septic shock following influenza A virus (IAV) pneumonia. Cupriavidus gilardii (C. gilardii) was identified in his blood and sputum samples. Through a literature review, we identified 31 reported cases of Cupriavidus infections. Clinical data, including demographic information, clinical characteristics, comorbidities, laboratory results, Cupriavidus species, treatment, and clinical outcomes, were collected. Results: Among these 32 patients (including our patient), 23 were male (71.9%) and 9 were female (28.1%). The median patient age was 32.5 (2.12–70) years. Most patients had relevant risk factors or comorbidities before Cupriavidus infection, including exposure to polluted environments and recent invasive procedures (68.9%). Among these cases, Cupriavidus pauculus was the most common strain, accounting for 56.3% of cases. The mortality rate was the highest for Cupriavidus pauculus infections. Conclusions: Cupriavidus is a rare opportunistic pathogen in patients with compromised immune function. Early identification of pathogen and timely treatment are crucial. When traditional microbiological detection methods encounter difficulties, gene sequencing can be used as an auxiliary diagnostic tool and can further predict drug resistance. Targeted anti-infection treatment is effective in most cases, but some severe infection cases may lead to death due to serious complications.
Full article
(This article belongs to the Section Bacterial Diseases)
►▼
Show Figures

Figure 1
Open AccessCase Report
Mycobacterium fortuitum: A Neglected Cause of Culture-Negative Prosthetic Valve Endocarditis and a Literature Review
by
Selen Şahin, İrem Tümkaya Kılınç, Eda Yüksel, Çağla Mehmet, Bedia Dinç and Emine Alp Meşe
Infect. Dis. Rep. 2026, 18(2), 23; https://doi.org/10.3390/idr18020023 - 13 Mar 2026
Abstract
Background/Objectives: Prosthetic valve endocarditis caused by non-tuberculous mycobacteria is a rare but serious condition and is often associated with delayed diagnosis due to initially negative routine blood cultures with late positivity after prolonged incubation. Mycobacterium fortuitum, a rapidly growing mycobacterium, is an
[...] Read more.
Background/Objectives: Prosthetic valve endocarditis caused by non-tuberculous mycobacteria is a rare but serious condition and is often associated with delayed diagnosis due to initially negative routine blood cultures with late positivity after prolonged incubation. Mycobacterium fortuitum, a rapidly growing mycobacterium, is an uncommon cause of endocarditis but may result in significant morbidity if not promptly identified. Methods: We report a 67-year-old man with prior cardiac surgery who presented 18 months later with recurrent fever, weight loss, and renal dysfunction. Initial blood cultures, echocardiography, and standard imaging were non-diagnostic. Ongoing clinical suspicion prompted extended mycobacterial cultures with prolonged incubation and molecular identification performed at a reference laboratory, which revealed M. fortuitum. Results: Antimicrobial susceptibility testing demonstrated susceptibility to amikacin, ciprofloxacin, and clarithromycin, and treatment was initiated with an amikacin-based combination regimen. The patient showed marked clinical and laboratory improvement, including resolution of fever and stabilization of renal function. Conclusions: This case highlights the diagnostic and therapeutic challenges of M. fortuitum prosthetic valve endocarditis and underscores the limitations of routine diagnostic methods in culture-negative endocarditis. It also emphasizes the importance of prolonged incubation and targeted microbiological workflows in suspected cases.
Full article
(This article belongs to the Special Issue Prevention, Diagnosis and Treatment of Healthcare-Associated Infections)
►▼
Show Figures

Figure 1
Open AccessReview
Trace Elements and Viral Infectious Diseases: Dual Roles in Pathogenesis and Immunity
by
Carla Mariana da Silva Medeiros, Michely da Silva Sousa, Lucas Hestevan Malta Alfredo, Jemmyson Romário de Jesus and Cícero Alves Lopes Júnior
Infect. Dis. Rep. 2026, 18(2), 22; https://doi.org/10.3390/idr18020022 - 10 Mar 2026
Abstract
Introduction: Trace elements such as zinc, selenium, iron, copper, and manganese play a vital role in human health—especially in how the immune system responds and how the body handles viral infections. These trace elements have complex and sometimes context-dependent effects: while they can
[...] Read more.
Introduction: Trace elements such as zinc, selenium, iron, copper, and manganese play a vital role in human health—especially in how the immune system responds and how the body handles viral infections. These trace elements have complex and sometimes context-dependent effects: while they can strengthen the body’s defenses, imbalances may promote viral replication and worsen tissue damage. Methods: Relevant articles discussed in this narrative review were identified through searches in major databases, including PubMed, Scopus, and Web of Science, primarily those published from 2020 onwards. Discussion: In this review, we examine key findings on how trace elements influence antioxidant defense, modulate viral replication, and regulate cytokine signaling, considering the context of innate immunity and the pathology of viral diseases. We discuss their impact on major infections such as HIV, viral hepatitis, and coronaviruses, highlighting how deficiencies or excesses of certain minerals can affect disease severity, immune responses, and clinical outcomes. The therapeutic use of trace element supplementation is also examined, emphasizing the importance of maintaining proper balance to avoid harmful effects. Conclusions: These findings contribute to a deeper understanding of the complex relationship between micronutrients and viral infections, which can inform the development of more effective prevention and treatment strategies. This review underscores the need for further clinical and experimental studies to define optimal levels of these elements in different health and disease scenarios.
Full article
(This article belongs to the Special Issue Viral Infectious Diseases: Epidemiology and Prevention Through Vaccination)
►▼
Show Figures

Figure 1
Open AccessCase Report
Streptococcus intermedius Septic Arthritis of the Acromioclavicular Joint with Periarticular Abscesses in an Elderly Man with Diabetes and Recent Canine Exposure: A Case Report and Literature Review
by
Gabriel A. Godart, Vidit Yadav, Elizabeth P. Wellings, Rupert O. Stanborough, Vincent C. Zummo, Bryan D. Springer, Ravi V. Durvasula and Sammer M. Elwasila
Infect. Dis. Rep. 2026, 18(2), 21; https://doi.org/10.3390/idr18020021 - 26 Feb 2026
Abstract
Background/Objectives: Streptococcus intermedius, a member of the Streptococcus anginosus group, is characterized by a marked propensity for abscess formation but only rarely causes native-joint septic arthritis. Involvement of the acromioclavicular (AC) joint is particularly uncommon. We describe a case of native AC
[...] Read more.
Background/Objectives: Streptococcus intermedius, a member of the Streptococcus anginosus group, is characterized by a marked propensity for abscess formation but only rarely causes native-joint septic arthritis. Involvement of the acromioclavicular (AC) joint is particularly uncommon. We describe a case of native AC joint septic arthritis due to S. intermedius in a patient with multiple predisposing factors and highlight diagnostic and management considerations. Methods: We report the clinical course of a 72-year-old man with poorly controlled type 2 diabetes mellitus who presented with progressive right shoulder pain, erythema, and swelling following recurrent minor skin abrasions from a newly adopted dog. Initial management for presumed inflammatory shoulder pathology included brief systemic corticosteroids and an ultrasound-guided intra-articular ketorolac injection. Magnetic resonance imaging (MRI) was performed after symptom progression. The patient underwent operative irrigation and debridement with collection of synovial fluid and deep tissue cultures. Blood cultures and transthoracic echocardiography were obtained to evaluate for systemic involvement. Results: MRI demonstrated multiloculated periarticular abscesses and osteolysis centered on the AC joint. Operative cultures yielded high colony counts of S. intermedius from synovial fluid and deep tissues. Blood cultures and echocardiography were negative. The patient required multiple operative debridements with irrigation, adjunctive local antibiotic therapy, and prolonged targeted β-lactam treatment. Clinical and radiographic improvement was achieved following surgical source control and antimicrobial therapy. Conclusions: Native AC joint septic arthritis due to S. intermedius is rare. Older age, uncontrolled diabetes, recent intra-articular intervention, and possible zoonotic inoculation from canine wound licking may represent contributory risk factors. Early imaging, prompt surgical source control, and guideline-concordant antimicrobial therapy are essential when bone and soft tissue involvement is present.
Full article
(This article belongs to the Section Bacterial Diseases)
►▼
Show Figures

Figure 1
Open AccessArticle
Post-COVID-19 Rabies Surveillance and Risk Factors in Rural Eastern Cape, South Africa: A One Health Perspective
by
Sithabile Moso, Laston Gonah, Mojisola Clara Hosu, Ntandazo Dlatu, Teke Apalata and Lindiwe Modest Faye
Infect. Dis. Rep. 2026, 18(2), 20; https://doi.org/10.3390/idr18020020 - 24 Feb 2026
Abstract
►▼
Show Figures
Background: Rabies remains a neglected zoonotic disease in South Africa, particularly in rural areas where surveillance weaknesses, behavioral gaps, and limited One Health coordination persist. Objectives: This study assessed rabies surveillance, behavioral risk factors, and system responsiveness in two rural Eastern Cape communities,
[...] Read more.
Background: Rabies remains a neglected zoonotic disease in South Africa, particularly in rural areas where surveillance weaknesses, behavioral gaps, and limited One Health coordination persist. Objectives: This study assessed rabies surveillance, behavioral risk factors, and system responsiveness in two rural Eastern Cape communities, with a focus on post-pandemic resilience within a One Health framework. Methods: A cross-sectional, community-based pilot study was conducted among 109 residents using structured questionnaires to collect data on demographics, rabies awareness, vaccination practices, and service disruptions. Descriptive, bivariate, and multivariate analyses identified predictors of dog-bite exposure and pet vaccination. Machine learning models (Decision Tree and Random Forest) were applied to explore risk hierarchies. A composite Surveillance Gap Index (SGI) was developed to integrate behavioral and systemic indicators. Results: While 88% of participants were aware of rabies, only 35% attended awareness campaigns. Dog-bite exposure affected 51% of households, with significantly higher risk among males (aOR = 4.33; p = 0.003). Education was positively associated with pet vaccination (aOR = 1.78). Despite 45% reporting COVID-19 disruptions, communities maintained high post-pandemic vaccination coverage (85.7%). Predictive models (AUC = 0.82–0.86) identified education, gender, awareness, and distance as key risk drivers. Conclusions: Integrating behavioral insights and predictive analytics into One Health strategies can strengthen rabies surveillance and support progress toward eliminating human rabies by 2030.
Full article

Figure 1
Open AccessArticle
Post-Exposure Prophylaxis Prescribing Practices in a Lyme Disease-Endemic Area
by
Eun Bin Lee, Anna Schotthoefer and Philip Whitfield
Infect. Dis. Rep. 2026, 18(1), 19; https://doi.org/10.3390/idr18010019 - 14 Feb 2026
Abstract
Background/Objectives: The 2020 Infectious Diseases Society of America (IDSA) guidelines recommend a single 200 mg dose of doxycycline within 72 h of tick removal after a high-risk bite for Lyme disease prophylaxis. However, limited data are available on prescribing practices related to this
[...] Read more.
Background/Objectives: The 2020 Infectious Diseases Society of America (IDSA) guidelines recommend a single 200 mg dose of doxycycline within 72 h of tick removal after a high-risk bite for Lyme disease prophylaxis. However, limited data are available on prescribing practices related to this recommendation in highly endemic Lyme disease areas. Methods: We conducted a retrospective chart review on adult patients (aged ≥ 18 years) who received a single dose of oral doxycycline for Lyme disease prevention for the period 2022–2024 within a rural Wisconsin health system. Patient and provider prescribing characteristics were evaluated. Manual data abstraction was performed on a random sample of 155 prescribing events to assess adherence to IDSA guidelines. Results: A total of 2404 prophylaxis prescriptions were identified; 44% were prescribed to older adults between 65 and 79 years of age, 54% were prescribed to males, and 66% were prescribed to patients living in rural areas. Prescriptions peaked in spring and summer months, consistent with the known seasonal trends in tick activity. Prescribing was distributed relatively evenly across provider types, with the majority (77%) of cases occurring in outpatient and urgent care settings. Upon manual abstraction, doxycycline was indicated in 12% with the remainder either classified as possibly indicated or not indicated due to suboptimal documentation and nonadherence. Conclusions: Our study identified high rates of incomplete documentation and uncertainty in guideline concordance in a Lyme-endemic health system, highlighting the opportunities to support evidence-based prescribing and to improve documentation practices.
Full article
(This article belongs to the Section Antimicrobial Stewardship and Resistance)
►▼
Show Figures

Figure 1
Open AccessArticle
Sickened by the Weather: Exploring the Climatic Impact on West Nile Virus (WNV) and Legionella pneumophila in Piedmont—A Retrospective Observational Study (2021–2024)
by
Paolo Valesella, Antonio Curtoni, Alessio Leone, Marco Iannaccone, Fabrizia Pittaluga, Elisa Zanotto, Alessandro Bondi, Rocco Francesco Rinaldo, Nour Shbaklo, Silvia Corcione, Simone Baldovino, Irene Cecchi, Elisa Menegatti, Paolo Solidoro and Cristina Costa
Infect. Dis. Rep. 2026, 18(1), 18; https://doi.org/10.3390/idr18010018 - 12 Feb 2026
Abstract
►▼
Show Figures
Background: Climate change represents a major global health challenge, with rising temperatures and altered precipitation patterns influencing the spread of infectious diseases. This study investigated the association between climatic factors (average temperature and precipitation) and the monthly proportion of laboratory-confirmed Legionella pneumophila serogroup
[...] Read more.
Background: Climate change represents a major global health challenge, with rising temperatures and altered precipitation patterns influencing the spread of infectious diseases. This study investigated the association between climatic factors (average temperature and precipitation) and the monthly proportion of laboratory-confirmed Legionella pneumophila serogroup 1 and West Nile Virus infections among clinically suspected patients in a large teaching hospital in Northern Italy. Methods: We retrospectively analyzed data from 2021 to 2024. The primary outcome was the monthly proportion of positive tests (standardized per 1000 clinically suspected patients) for Legionella pneumophila serogroup 1 (urinary antigen) and West Nile Virus (serology). Associations with climatic variables were assessed using linear and multivariate regression models, as well as Generalized Additive Models (GAMs). Seasonal effects were evaluated through ANOVA. Results: For Legionella pneumophila, precipitation was not significantly associated with the proportion of positive tests (p = 0.1438; R2 = 0.049). In contrast, average temperature was a significant predictor: each 1 °C increase was associated with +0.52 positive cases per 1000 tested patients (p = 0.000283; R2 = 0.267). Multivariate models confirmed temperature as the dominant factor. For West Nile Virus, precipitation showed no meaningful effect (p = 0.914). However, average temperature demonstrated a significant positive association with the proportion of positive cases (p = 0.00293; coefficient = 9.33), with seasonal analysis highlighting a marked summer peak (mean = 399.68 positive cases per 1000 tested; p = 0.00653). Conclusions: Our findings underline the predominant role of temperature over precipitation in driving the burden of both Legionella pneumophila and West Nile Virus infections among hospitalized patients. These results strengthen the evidence that the life cycles of these pathogens are tightly climate-dependent. Developing effective adaptation strategies is essential to mitigate climate-related health risks.
Full article

Figure 1
Open AccessCase Report
Prosthetic-Valve Endocarditis with Discordant Isolates: A Case Report and a Review of the Literature
by
Raffaele Ferri, Francesco Mucedola, Marcella Conserva, Jacopo Vecchiet and Katia Falasca
Infect. Dis. Rep. 2026, 18(1), 17; https://doi.org/10.3390/idr18010017 - 12 Feb 2026
Abstract
Prosthetic-valve endocarditis (PVE) represents one of the most serious forms of infective endocarditis, marked by high mortality and considerable management complexity. The 2023 European Society of Cardiology (ESC) Guidelines emphasise the diagnostic centrality of repeatedly positive blood cultures. Nonetheless, a significant area of
[...] Read more.
Prosthetic-valve endocarditis (PVE) represents one of the most serious forms of infective endocarditis, marked by high mortality and considerable management complexity. The 2023 European Society of Cardiology (ESC) Guidelines emphasise the diagnostic centrality of repeatedly positive blood cultures. Nonetheless, a significant area of uncertainty remains regarding the diagnostic and prognostic value of cultures from explanted prosthetic valves—particularly in centres lacking access to molecular diagnostics. Case Presentation: We report a case of prosthetic-valve endocarditis on a bioprosthesis, in which repeated blood-culture sets yielded Streptococcus acidominimus, whereas culture of the explanted valve revealed Staphylococcus warnerii. The patient received six weeks of intravenous vancomycin, with treatment tailored according to the patient’s clinical and laboratory parameters and in alignment with international endocarditis guidelines, obtaining a clear clinical and laboratory improvement. Discussion: The literature reports that discordance between blood-culture and valve-culture results in infective endocarditis may range from approximately 10% to 29%, attributable to contamination, biofilm formation or polymicrobial infection. In our case, management guided by the microorganism repeatedly isolated from blood cultures proved effective and aligned with the 2023 European Society of Cardiology (ESC) guidelines. The case underlines the importance of a multidisciplinary team and an integrated interpretation of microbiological, clinical and surgical data. Conclusions: Infective endocarditis with discordant isolates presents a complex diagnostic challenge. The etiological diagnosis must rely primarily on the results of blood cultures, whereas valve culture plays a complementary role—useful more for prognostic stratification than for initial diagnostic purposes. A multidisciplinary approach and a critical interpretation of microbiological findings are essential to optimise therapeutic management and improve patient outcomes.
Full article
(This article belongs to the Section Bacterial Diseases)
Open AccessSystematic Review
Efficacy and Safety of Minocycline-Containing Bismuth Quadruple Therapies Versus Standard First-Line Bismuth Quadruple Therapies for Helicobacter pylori Eradication: A Systematic Review and Meta-Analysis
by
Hakim Ullah Wazir, Abdul Muqeet Khuram, I M Khalid Reza, Hafsa Ajmal, Hafsa Parveen, Zeeshan Ahmed, Yousra Iftequar, Noora Inam, Ilyas Muhammad Sulaiman, Nayanika Tummala, Hafiz Muhammad Moaaz Sajid, Anum Zia Khan and Ussama Shafaqat
Infect. Dis. Rep. 2026, 18(1), 16; https://doi.org/10.3390/idr18010016 - 6 Feb 2026
Abstract
►▼
Show Figures
Background: Growing antibiotic resistance and the limited availability of key components in standard Helicobacter pylori treatments have driven the search for effective alternatives. Minocycline, with its broad-spectrum activity and favorable pharmacokinetics, has emerged as a promising substitute. This meta-analysis compares the safety and
[...] Read more.
Background: Growing antibiotic resistance and the limited availability of key components in standard Helicobacter pylori treatments have driven the search for effective alternatives. Minocycline, with its broad-spectrum activity and favorable pharmacokinetics, has emerged as a promising substitute. This meta-analysis compares the safety and efficacy of minocycline-containing bismuth quadruple therapy (MBQT) to conventional first-line BQT regimens, incorporating data from the recent study by Lin et al. Methods: The inclusion criteria were randomized controlled trials (RCTs) with a target population of both treatment-naïve and previously treated patients diagnosed with Helicobacter pylori (H. pylori) infection. The intervention received by eligible patients was a minocycline–bismuth quadruple therapy (MBQT) regimen containing bismuth, minocycline, proton pump inhibitors (PPI), and any additional antibiotic with a minimum period of 2 weeks of administration. We excluded study designs other than RCT and clinical trials that include patients without confirmed H. pylori infection, animal populations, in vitro experiments, and reports of other outcomes that did not include a minimum intervention duration of 2 weeks. A comprehensive literature search was conducted on PubMed, EMBASE, Cochrane Library, and ScienceDirect from inception to 20 May 2025. After screening via Rayyan, data were extracted on an Excel spreadsheet. Quality was assessed using the Cochrane RoB 2.0 tool. Eligible randomized controlled trials (RCTs) were included and analyzed using RevMan 5.4. Outcomes assessed were intention-to-treat and per-protocol eradication rates. Adverse effects were compared among therapies. A random-effects model was used; an I2 < 50% and p-value < 0.05 indicated homogeneity and significant results respectively. Results: Five RCTs with 7 interventions involving 2812 patients were included. The pooled odds ratio (OR) for MBQT in intention-to-treat (ITT) analysis was 1.25 (95% CI: 0.96–1.61), showing a non-significant trend. No heterogeneity was detected (I2 = 0.0%). In the modified ITT (mITT) analysis (2 studies), MBQT showed higher eradication (OR: 1.70, 95% CI: 0.00–1042.90), but wide CI and high heterogeneity (I2 = 70.7%) limited interpretation. All studies were included in the per-protocol (PP) analysis, which showed a statistically significant improvement with MBQT (OR: 1.67, 95% CI: 1.14–2.45) and low heterogeneity (I2 = 5.2%), suggesting consistent results. Although not statistically significant, MBQT was associated with a slightly lower rate of adverse events compared to standard therapy (OR: 0.81, 95% CI: 0.59–1.12). I2 = 50.6% showed moderate heterogeneity in safety outcomes. Discussion: the number of included RCTs was modest, with only five studies meeting eligibility criteria, and only two contributing to the modified intention-to-treat analysis. The risk-of-bias assessment showed variation in methodological quality across the included studies. Several studies exhibited high risk judgments in critical domains. particularly randomization, deviations from intervention, and selective reporting. Patients who completed the treatment benefited more from MBQT, which also had a comparable safety profile to conventional BQT regimens. In the treatment of H. pylori infection, MBQT may be considered a safe alternative for first-line treatment.
Full article

Figure 1
Open AccessReview
Atypical Presentations in Melioidosis: A Case-Based Review from Endemic Regions
by
Saurav Jyoti Patgiri, Anukalpa Saikia, Sushmita Yadav, Md. Atique Ahmed, Luna Adhikari, Chimanjita Phukan, Chiranjay Mukhopadhyay and Harpreet Kaur
Infect. Dis. Rep. 2026, 18(1), 15; https://doi.org/10.3390/idr18010015 - 3 Feb 2026
Abstract
Background: Melioidosis, caused by Burkholderia pseudomallei, is a severe and often underdiagnosed infection endemic to South Asia, Southeast Asia, and northern Australia. While pneumonia and sepsis are the classical presentations, the disease is increasingly recognized for its diverse and atypical clinical manifestations.
[...] Read more.
Background: Melioidosis, caused by Burkholderia pseudomallei, is a severe and often underdiagnosed infection endemic to South Asia, Southeast Asia, and northern Australia. While pneumonia and sepsis are the classical presentations, the disease is increasingly recognized for its diverse and atypical clinical manifestations. Objective: The objective is to improve diagnostic accuracy and increase clinical awareness in both endemic and non-endemic settings by reviewing and classifying atypical presentations of melioidosis that have been documented in the literature. Methods: A narrative, case-based review was conducted using 238 published case reports and series from endemic and transitional regions during the period from 2000 to 2025. Cases with non-respiratory presentations or anatomical locations not commonly linked to melioidosis were classified as atypical. Clinical syndromes were used to classify the extracted cases, and common patterns in presentation, diagnosis, and outcome were examined. Results: One hundred and sixty published articles were included after a full text review. The most frequent atypical presentations included neurological involvement (e.g., brain abscess, encephalomyelitis), musculoskeletal infections (osteomyelitis, myositis), thyroid abscess, tubo-ovarian abscess, and dermatologic manifestations such as erythema nodosum. Imported and pediatric cases were also found. Numerous cases were misidentified as cancer, fungal infections, or tuberculosis. Among risk factors, diabetes mellitus was the most prevalent. Non-specific symptoms, a lack of laboratory capacity, and incorrect pathogen identification frequently resulted in delays in diagnosis. Conclusions: In endemic areas, melioidosis should be taken into account when making a differential diagnosis of a variety of clinical syndromes, especially in patients who have diabetes or have had relevant environmental exposure. Poor outcomes and diagnostic delays are greatly exacerbated by atypical presentations. Improving diagnostic capabilities and raising awareness are crucial to lessening the worldwide burden of this often ignored but potentially deadly infection.
Full article
(This article belongs to the Special Issue Review on Infectious Diseases)
Open AccessArticle
Invasive Fusariosis: Unusual Cases over 10 Years in a Tertiary Care Hospital and a Review of the Literature from Saudi Arabia
by
Hassan Almarhabi, Abdulmajeed Sarhan, Murad Essatari and Hassan Huwait
Infect. Dis. Rep. 2026, 18(1), 14; https://doi.org/10.3390/idr18010014 - 26 Jan 2026
Abstract
►▼
Show Figures
Background/Objectives: Fusarium species are recognized as difficult-to-treat opportunistic pathogens due to extensive antifungal resistance and high mortality rates. Variability in its incidence and outcomes exists across different countries and centers. Large studies on Fusarium species are lacking in Saudi Arabia, with most
[...] Read more.
Background/Objectives: Fusarium species are recognized as difficult-to-treat opportunistic pathogens due to extensive antifungal resistance and high mortality rates. Variability in its incidence and outcomes exists across different countries and centers. Large studies on Fusarium species are lacking in Saudi Arabia, with most previous publications being case reports. We describe all cases of invasive fusariosis identified at a tertiary center during a 10-year period and review previous reports in the country. Methods: A retrospective search of hospital records and the microbiology database was conducted to identify cases of invasive fusariosis among patients admitted during 2016–2025 at King Abdulaziz Medical City, Jeddah, Saudi Arabia. Results: Three cases of invasive fusariosis occurring over a 10-year period were identified. All cases occurred in the last three years of the study period. The incidence during those three years was 0.4 cases per 10,000 admissions per year. Clinical manifestations were fungemia in two immunocompetent patients and ulcers progressing to osteomyelitis in an immunocompromised patient. None of the patients progressed to death within 30 days of diagnosis. Conclusions: Data on Fusarium species are scarce in Saudi Arabia. Additional studies are required to better understand differences in invasive fusariosis between countries.
Full article

Figure 1
Highly Accessed Articles
Latest Books
E-Mail Alert
News
Topics
Topic in
Infectious Disease Reports, Insects, IJERPH, Pathogens, TropicalMed, Zoonotic Diseases
Vector-Borne Disease Spatial Epidemiology, Disease Ecology, and Zoonoses
Topic Editors: Chad L. Cross, Louisa Alexandra MessengerDeadline: 31 December 2026
Topic in
IJERPH, TropicalMed, Microorganisms, Infectious Disease Reports, Pathogens
Genetic, Environmental, and Climatic Drivers of Emerging Arboviruses and Public Health Implications
Topic Editors: André Ricardo Ribas Freitas, Pedro María Alarcón-Elbal, Luciano Pamplona de Góes CavalcantiDeadline: 20 January 2027
Topic in
Diseases, Epidemiologia, Infectious Disease Reports, Medicina, TropicalMed
Surveillance Systems and Predictive Analytics for Epidemics
Topic Editors: Georgia Kourlaba, Elisavet StavropoulouDeadline: 31 January 2027

Special Issues
Special Issue in
Infectious Disease Reports
Prevention, Diagnosis and Treatment of Healthcare-Associated Infections
Guest Editor: Emine Alp MeşeDeadline: 31 May 2026
Special Issue in
Infectious Disease Reports
Challenges in the Management of Onychomycosis and Other Superficial Fungal Infections
Guest Editor: Aditya K. GuptaDeadline: 30 June 2026
Special Issue in
Infectious Disease Reports
Infections in Vulnerable Populations
Guest Editors: Botond Lakatos, Francesco Di GennaroDeadline: 30 June 2026
Special Issue in
Infectious Disease Reports
Review on Infectious Diseases
Guest Editor: Carlo TasciniDeadline: 1 July 2026